In today’s dynamic healthcare environment, denial management in healthcare billing is more critical than ever. Efficient denial management not only optimizes cash flow but also strengthens patient satisfaction and organizational stability. Despite technological advancements and evolving payer rules, healthcare providers continue to face challenges with claim denials that directly affect their bottom line. At Allzone, we […]
Important Points: The CO-31 denial is one of the easiest claim rejections to avoid in medical billing. Most of the cases are caused by simple mistakes in demographics or eligibility that can be fixed with better front-end processes. Keep in mind: • Check eligibility early • Make sure the patient data is correct • Check […]
Providers and revenue cycle teams still have a lot of trouble with claims that are denied in today’s healthcare system. Repeated denials not only slow down payments, but they also make it harder for healthcare organizations to do their jobs and hurt their overall financial health. Root cause analysis helps you find and fix the […]
If you ask any experienced revenue cycle manager what truly determines the financial health of a healthcare organization, the answer is rarely coding or charge entry alone. The real difference often lies in one specific operational area — insurance follow-ups. Claims are submitted every day. Payments are expected every day. But revenue is actually realized […]
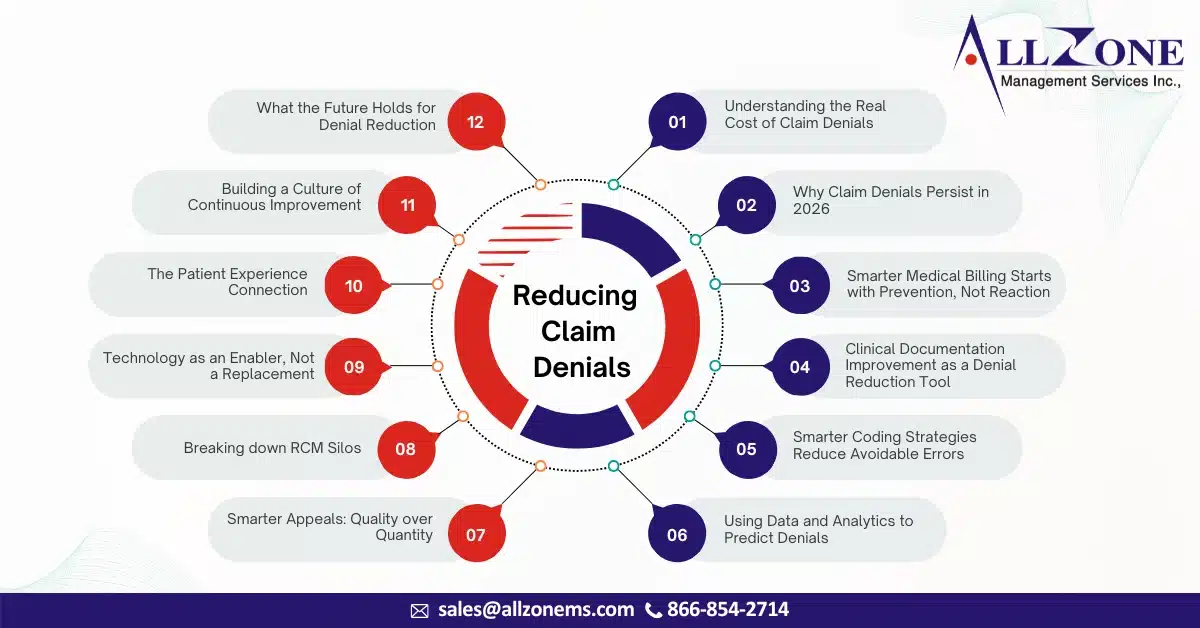
In 2026, claim denials are no longer viewed as an unavoidable part of healthcare operations—they are increasingly seen as a preventable revenue leak. As margins tighten, payer scrutiny intensifies, and patient expectations rise, healthcare organizations are under more pressure than ever to get billing right the first time. Yet, despite advancements in technology and data […]
Medical claim denials continue to pose a serious challenge for healthcare providers striving to maintain steady cash flow and financial stability. As payer policies become increasingly complex, documentation standards tighten, and reimbursement models evolve, even a minor oversight in billing or coding can result in delayed payments or lost revenue. Effective denial management in medical […]
As the year comes to a close, healthcare organizations feel the same pressure they always do: closing out accounts, speeding up collections, settling outstanding claims, and getting rid of operational bottlenecks before January 1st. The last three months of the year are often the most important for a company’s financial health. What happens now will […]
Accurate modifier usage is one of the most important elements in achieving clean claim submissions and full reimbursement in surgical billing. Among the lesser-used but extremely important surgical modifiers is Modifier 81 – Minimum Assistant Surgeon. Many practices overlook or misuse this modifier, leading to preventable denials, delayed payments, and compliance issues. This comprehensive guide […]
Introduction In medical billing, modifiers play a vital role in explaining the circumstances under which a service or procedure was performed. One such important modifier is Modifier 76, which helps billers and coders indicate when a repeat procedure or service is performed by the same physician or qualified healthcare professional. Accurate use of Modifier 76 […]
In the complex world of medical billing, claim denials are one of the biggest challenges healthcare providers face. Among them, CO-97 denial code is one of the most frequent and confusing denials providers encounter. A denied claim not only disrupts cash flow but also leads to additional administrative costs and potential compliance risks. To minimize […]